- Diabetes, obesity and metabolism
- Efficacy of Gemigliptin Add-on to Dapagliflozin and Metformin in Type 2 Diabetes Patients: A Randomized, Double-Blind, Placebo-Controlled Study (SOLUTION)
-
Byung Wan Lee, KyungWan Min, Eun-Gyoung Hong, Bon Jeong Ku, Jun Goo Kang, Suk Chon, Won-Young Lee, Mi Kyoung Park, Jae Hyeon Kim, Sang Yong Kim, Keeho Song, Soon Jib Yoo
-
Endocrinol Metab. 2023;38(3):328-337. Published online June 28, 2023
-
DOI: https://doi.org/10.3803/EnM.2023.1688
-
-
 Abstract Abstract
 PDF PDF Supplementary Material Supplementary Material PubReader PubReader  ePub ePub
- Background
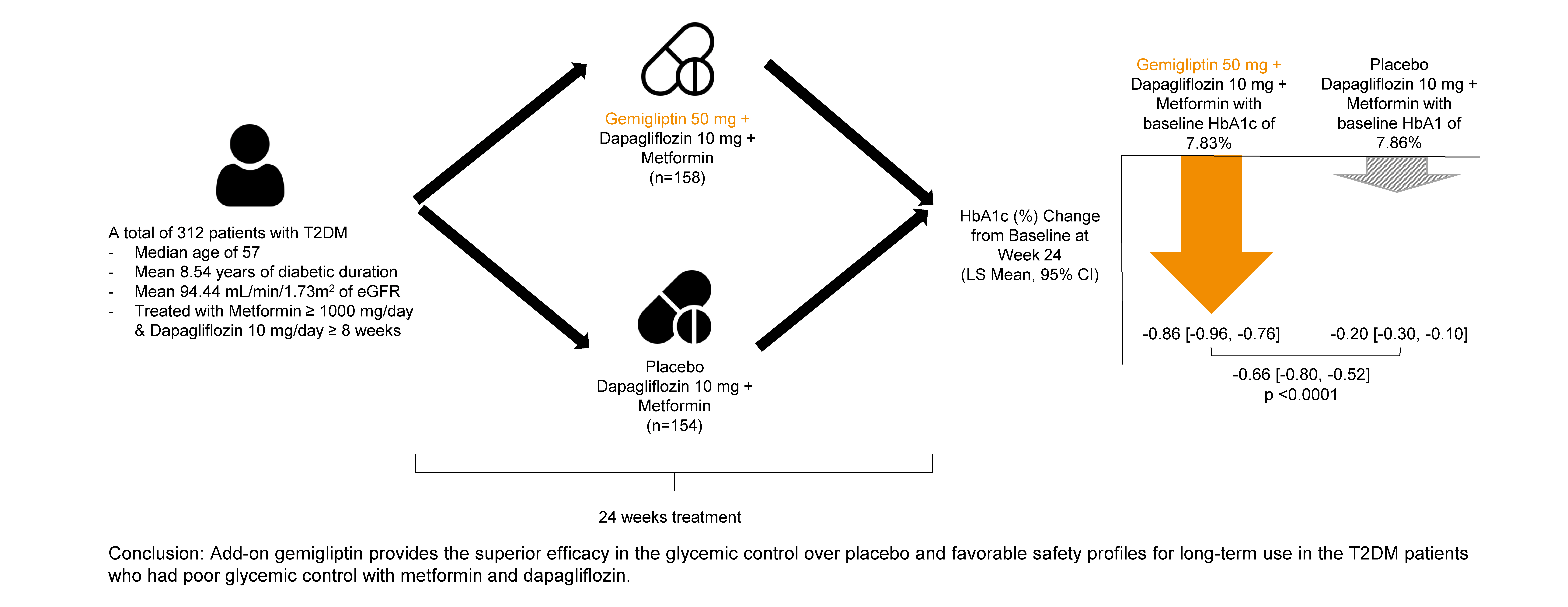
This study evaluated the efficacy and safety of add-on gemigliptin in patients with type 2 diabetes mellitus (T2DM) who had inadequate glycemic control with metformin and dapagliflozin.
Methods
In this randomized, placebo-controlled, parallel-group, double-blind, phase III study, 315 patients were randomized to receive either gemigliptin 50 mg (n=159) or placebo (n=156) with metformin and dapagliflozin for 24 weeks. After the 24-week treatment, patients who received the placebo were switched to gemigliptin, and all patients were treated with gemigliptin for an additional 28 weeks.
Results
The baseline characteristics were similar between the two groups, except for body mass index. At week 24, the least squares mean difference (standard error) in hemoglobin A1c (HbA1c) changes was –0.66% (0.07) with a 95% confidence interval of –0.80% to –0.52%, demonstrating superior HbA1c reduction in the gemigliptin group. After week 24, the HbA1c level significantly decreased in the placebo group as gemigliptin was administered, whereas the efficacy of HbA1c reduction was maintained up to week 52 in the gemigliptin group. The safety profiles were similar: the incidence rates of treatment-emergent adverse events up to week 24 were 27.67% and 29.22% in the gemigliptin and placebo groups, respectively. The safety profiles after week 24 were similar to those up to week 24 in both groups, and no new safety findings, including hypoglycemia, were noted.
Conclusion
Add-on gemigliptin was well tolerated, providing comparable safety profiles and superior efficacy in glycemic control over placebo for long-term use in patients with T2DM who had poor glycemic control with metformin and dapagliflozin.
- Glucocorticoid-Induced Diabetes Mellitus: An Important but Overlooked Problem
-
Sunghwan Suh, Mi Kyoung Park
-
Endocrinol Metab. 2017;32(2):180-189. Published online May 29, 2017
-
DOI: https://doi.org/10.3803/EnM.2017.32.2.180
-
-
15,383
View
-
595
Download
-
108
Web of Science
-
117
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
Glucocorticoids are widely used as potent anti-inflammatory and immunosuppressive drugs to treat a wide range of diseases. However, they are also associated with a number of side effects, including new-onset hyperglycemia in patients without a history of diabetes mellitus (DM) or severely uncontrolled hyperglycemia in patients with known DM. Glucocorticoid-induced diabetes mellitus (GIDM) is a common and potentially harmful problem in clinical practice, affecting almost all medical specialties, but is often difficult to detect in clinical settings. However, scientific evidence is lacking regarding the effects of GIDM, as well as strategies for prevention and treatment. Similarly to nonsteroid-related DM, the principles of early detection and risk factor modification apply. Screening for GIDM should be considered in all patients treated with medium to high doses of glucocorticoids. Challenges in the management of GIDM stem from wide fluctuations in postprandial hyperglycemia and the lack of clearly defined treatment protocols. Together with lifestyle measures, hypoglycemic drugs with insulin-sensitizing effects are indicated. However, insulin therapy is often unavoidable, to the point that insulin can be considered the drug of choice. The treatment of GIDM should take into account the degree and pattern of hyperglycemia, as well as the type, dose, and schedule of glucocorticoid used. Moreover, it is essential to instruct the patient and/or the patient's family about how to perform the necessary adjustments. Prospective studies are needed to answer the remaining questions regarding GIDM. -
Citations
Citations to this article as recorded by 
- Clinical Study
- Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development of Type 2 Diabetes Mellitus
-
Sunghwan Suh, Mi Yeon Kim, Soo Kyoung Kim, Kyu Yeon Hur, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
-
Endocrinol Metab. 2016;31(1):134-141. Published online March 16, 2016
-
DOI: https://doi.org/10.3803/EnM.2016.31.1.134
-
-
3,839
View
-
44
Download
-
7
Web of Science
-
6
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Incretin hormone levels as a predictor of type 2 diabetes mellitus have not been fully investigated. Therefore, we measured incretin hormone levels to examine the relationship between circulating incretin hormones, diabetes, and future diabetes development in this study. MethodsA nested case-control study was conducted in a Korean cohort. The study included the following two groups: the control group (n=149), the incident diabetes group (n=65). Fasting total glucagon-like peptide-1 (GLP-1) and total glucose-dependent insulinotropic peptide (GIP) levels were measured and compared between these groups. ResultsFasting total GIP levels were higher in the incident diabetes group than in the control group (32.64±22.68 pmol/L vs. 25.54±18.37 pmol/L, P=0.034). There was no statistically significant difference in fasting total GLP-1 levels between groups (1.14±1.43 pmol/L vs. 1.39±2.13 pmol/L, P=0.199). In multivariate analysis, fasting total GIP levels were associated with an increased risk of diabetes (odds ratio, 1.005; P=0.012) independent of other risk factors. ConclusionFasting total GIP levels may be a risk factor for the development of type 2 diabetes mellitus. This association persisted even after adjusting for other metabolic parameters such as elevated fasting glucose, hemoglobin A1c, and obesity in the pre-diabetic period.
-
Citations
Citations to this article as recorded by  - Mendelian randomization analyses suggest a causal role for circulating GIP and IL-1RA levels in homeostatic model assessment-derived measures of β-cell function and insulin sensitivity in Africans without type 2 diabetes
Karlijn A. C. Meeks, Amy R. Bentley, Themistocles L. Assimes, Nora Franceschini, Adebowale A. Adeyemo, Charles N. Rotimi, Ayo P. Doumatey
Genome Medicine.2023;[Epub] CrossRef - Glucose- and Bile Acid-Stimulated Secretion of Gut Hormones in the Isolated Perfused Intestine Is Not Impaired in Diet-Induced Obese Mice
Jenna E. Hunt, Jens J. Holst, Sara L. Jepsen
Frontiers in Endocrinology.2022;[Epub] CrossRef - Combined treatment with a gastric inhibitory polypeptide receptor antagonist and a peptidyl peptidase-4 inhibitor improves metabolic abnormalities in diabetic mice
Fei Yang, Shan Dang, Hongjun LV, Bingyin Shi
Journal of International Medical Research.2021; 49(1): 030006052098566. CrossRef - Elevated levels of fasting serum GIP may be protective factors for diabetic retinopathy in type 2 diabetes mellitus
LingHong Huang, JingXiong Zhou, Bo Liang, HuiBin Huang, LiangYi Li
International Journal of Diabetes in Developing Countries.2021; 41(4): 543. CrossRef - Enteroendocrine K and L cells in healthy and type 2 diabetic individuals
Tina Jorsal, Nicolai A. Rhee, Jens Pedersen, Camilla D. Wahlgren, Brynjulf Mortensen, Sara L. Jepsen, Jacob Jelsing, Louise S. Dalbøge, Peter Vilmann, Hazem Hassan, Jakob W. Hendel, Steen S. Poulsen, Jens J. Holst, Tina Vilsbøll, Filip K. Knop
Diabetologia.2018; 61(2): 284. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef
- Obesity and Metabolism
- Sex Factors in the Metabolic Syndrome as a Predictor of Cardiovascular Disease
-
Sunghwan Suh, Jongha Baek, Ji Cheol Bae, Kyoung-Nyoun Kim, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
-
Endocrinol Metab. 2014;29(4):522-529. Published online December 29, 2014
-
DOI: https://doi.org/10.3803/EnM.2014.29.4.522
-
-
4,714
View
-
37
Download
-
16
Web of Science
-
17
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader
- Background
Metabolic syndrome (MetS) is a condition characterized by a cluster of metabolic disorders and is associated with increased risk of cardiovascular disease (CVD). This study analyzed data from the Korean Health and Genome Study to examine the impact of MetS on CVD. MethodsA total of 8,898 subjects (4,241 males and 4,657 females), 40 to 69 years of age, were enrolled and evaluated for the development of new onset CVD from 2001 to 2012 (median 8.1 years of follow-up). ResultsThe prevalence of MetS at baseline was 22.0% (932/4,241) and 29.7% (1,383/4,657) in males and females, respectively. MetS was associated with increased risk of coronary heart disease (CHD; hazard ratio [HR], 1.818; 95% confidence interval [CI], 1.312 to 2.520 in males; HR, 1.789; 95% CI, 1.332 to 2.404 in females) and CVD (HR, 1.689; 95% CI, 1.295 to 2.204 in males; HR, 1.686; 95% CI, 1.007 to 2.192 in females). Specifically, MetS was associated with risk of future stroke in females only (HR, 1.486; 95% CI, 1.007 to 2.192). Among MetS components, abdominal obesity and hypertension were independent predictors of both CHD and CVD. In addition, a higher number of MetS components correlated with higher CVD risk. ConclusionMetS is a significant risk factor for the development of CVD although its impact varies between sexes.
-
Citations
Citations to this article as recorded by  - Cardiovascular age of workers with different employment categories
Byung-Kook Lee, Jaeouk Ahn, Nam-Soo Kim, Jungsun Park, Yangho Kim
Archives of Environmental & Occupational Health.2022; 77(3): 243. CrossRef - Effects of Anthocyanin-rich Berries on the Risk of Metabolic Syndrome: A Systematic Review and Meta-analysis
Mikkel Roulund Wilken, Max Norman Tandrup Lambert, Christine Bodelund Christensen, Per Bendix Jeppesen
Review of Diabetic Studies.2022; 18(1): 42. CrossRef - Rate and risk factors of metabolic components and component combinations according to hypertension status in Tibetans in a cross-sectional study
Jihong Hu, Brian Thompson, Shuxia Wang, Minhao Guo, Chunjuan Yan, Fengfeng Ding, Peng Guo, Li Chen, Zhuoma Cao, Jianzong Wang
Medicine.2022; 101(43): e31320. CrossRef - Gender differences in changes in metabolic syndrome status and its components and risk of cardiovascular disease: a longitudinal cohort study
Azra Ramezankhani, Fereidoun Azizi, Farzad Hadaegh
Cardiovascular Diabetology.2022;[Epub] CrossRef - The Association of Metabolic Syndrome with the development of cardiovascular disease among Kazakhs in remote rural areas of Xinjiang, China: a cohort study
Wenwen Yang, Shuxia Guo, Haixia Wang, Yu Li, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Yanpeng Song, Changjing Li, Zhuo Ma, Rulin Ma, Jia He
BMC Public Health.2021;[Epub] CrossRef - Serum Arylsulfatase and Acid Phosphatase Activity in Patients with Metabolic Syndrome as a Result of Oxidative Damage to Lysosomes
Dorota M. Olszewska-Słonina
Protein & Peptide Letters.2021; 28(11): 1246. CrossRef - Validation of Risk Prediction Models for Atherosclerotic Cardiovascular Disease in a Prospective Korean Community-Based Cohort
Jae Hyun Bae, Min Kyong Moon, Sohee Oh, Bo Kyung Koo, Nam Han Cho, Moon-Kyu Lee
Diabetes & Metabolism Journal.2020; 44(3): 458. CrossRef - The Prevalence of Obesity and Metabolic Syndrome in the Korean Military Compared with the General Population
Jung Hwan Lee, Da Hea Seo, Min Jung Nam, Geon Hui Lee, Dong Hee Yang, Min Joo Lee, Ung-Rim Choi, Seongbin Hong
Journal of Korean Medical Science.2018;[Epub] CrossRef - Relationship between serum bilirubin levels and cardiovascular disease
Sunghwan Suh, Young Rak Cho, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee, Christian Herder
PLOS ONE.2018; 13(2): e0193041. CrossRef - Comparison Between Metabolic Syndrome and the Framingham Risk Score as Predictors of Cardiovascular Diseases Among Kazakhs in Xinjiang
Wenwen Yang, Rulin Ma, Xianghui Zhang, Heng Guo, Jia He, Lei Mao, Lati Mu, Yunhua Hu, Yizhong Yan, Jiaming Liu, Jiaolong Ma, Shugang Li, Yusong Ding, Mei Zhang, Jingyu Zhang, Shuxia Guo
Scientific Reports.2018;[Epub] CrossRef - Impact of interactions among metabolic syndrome components on the development of cardiovascular disease among Kazakhs in Xinjiang
Wenwen Yang, Xiang Gao, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jia He, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Shugang Li, Yusong Ding, Mei Zhang, Rulin Ma, Shuxia Guo, Mahesh Narayan
PLOS ONE.2018; 13(10): e0205703. CrossRef - Prediction of cardiovascular disease in Korean population: based on health risk appraisal of national health screening program
Jae Moon Yun, Tae Gon Yoo, Seung-Won Oh, Be Long Cho, Eunyoung Kim, Insob Hwang
Journal of the Korean Medical Association.2017; 60(9): 746. CrossRef - Metabolic Syndrome Is a Strong Risk Factor for Minor Ischemic Stroke and Subsequent Vascular Events
Guang-Sheng Wang, Dao-Ming Tong, Xiao-Dong Chen, Tong-Hui Yang, Ye-Ting Zhou, Xiao-Bo Ma, Gianpaolo Reboldi
PLOS ONE.2016; 11(8): e0156243. CrossRef - Metabolic syndrome related to cardiovascular events in a 10-year prospective study
Laura Kazlauskienė, Jūratė Butnorienė, Antanas Norkus
Diabetology & Metabolic Syndrome.2015;[Epub] CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Impact of Cadmium Exposure on the Association between Lipopolysaccharide and Metabolic Syndrome
Seung Han, Kyoung Ha, Ja Jeon, Hae Kim, Kwan Lee, Dae Kim
International Journal of Environmental Research and Public Health.2015; 12(9): 11396. CrossRef - Heat Killed Lactobacillus reuteri GMNL-263 Reduces Fibrosis Effects on the Liver and Heart in High Fat Diet-Hamsters via TGF-β Suppression
Wei-Jen Ting, Wei-Wen Kuo, Dennis Hsieh, Yu-Lan Yeh, Cecilia-Hsuan Day, Ya-Hui Chen, Ray-Jade Chen, Viswanadha Padma, Yi-Hsing Chen, Chih-Yang Huang
International Journal of Molecular Sciences.2015; 16(10): 25881. CrossRef
- A Case of Graves' Disease Presented as Generalized Seizure Attack.
-
So Young Park, Su Kyoung Park, Sung Hwan Suh, Duk Kyu Kim, Sang Ho Kim, Mi Kyoung Park, Song Yee Han, Seung Hee Ryu, Su Mi Woo, Sung Woo Lee, Neul Bom Yoon
-
Endocrinol Metab. 2012;27(2):142-146. Published online June 20, 2012
-
DOI: https://doi.org/10.3803/EnM.2012.27.2.142
-
-
 Abstract Abstract
 PDF PDF
- Hyperthyroidism is diagnosed when a patient is presented with typical symptoms, such as weight loss, palpitation, and hand tremor. However, early diagnosis is difficult in elders, because they have no typical symptoms, but only cardiovascular or muscular symptoms. In hyperthyroidism, there are often with neurologic changes, leading to various neurologic symptoms. Generalized or focal seizures are rarely reported in thyrotoxicosis and thyrotoxic crisis. Further, cases of hyperthyroidism presented as generalized seizure attack are extremely rare. We report a case of hyperthyroidism. A patient is presented at the hospital with mental change, as well as generalized seizure, who was finally diagnosed to have Graves' disease. A 56-year-old male was admitted to the hospital because of mental change with generalized seizure attack. Initial neurologic evaluations, including a brain magnetic resonance imaging and electroencephalogram proved to be normal. But, thyroid function test showed abnormal results. We diagnosed him as Graves' disease and prescribed anti-thyroid drug. Thereafter, there has been no recurrence of neurologic symptoms for 12 months.
- A Case of Primary Hyperparathyroidism with Rapid Regression of a Brown Tumor after Parathyroidectomy.
-
Ji Young Mok, Ha Yeon Kim, Hsing Chien Ter, Sang Ock Kim, Dong Kyun Kim, Ji Sun Han, So Young Park, Sa Rah Lee, Mi Kyoung Park, Duk Kyu Kim
-
J Korean Endocr Soc. 2010;25(1):50-55. Published online March 1, 2010
-
DOI: https://doi.org/10.3803/jkes.2010.25.1.50
-
-
 Abstract Abstract
 PDF PDF
- Primary hyperparathyroidism is mainly caused by parathyroid adenoma (85%) and is characterized by hypercalcemia, osteoporosis, renal stones, and gastrointestinal and neurological disorders. Because of improvements in blood analysis over the last two decades, primary hyperparathyroidism is typically diagnosed early and asymptomatically. A rare clinical manifestations of primary hyperparathyroidism, brown tumors (osteitis fibrosa cystica), are osteolytic lesions resulting from long-term hyperparathyroidism. Radiologically, it is difficult to distinguish a brown tumor from plasmacytoma, multiple myeloma, or bone metastasis. We report a case of a 44-year-old man with primary hyperparathyroidism that caused a large brown tumor (11 x 5 x 8 cm) that mimicked plasmacytoma or cancer metastasis on pelvic magnetic resonance imaging. After a bone biopsy report that was highly suggestive of a brown tumor, serum calcium and intact parathyroid hormone levels were determined. The lesion was ultimately diagnosed as a brown tumor and a parathyroidectomy was performed. After 1 year, the lesion has nearly regressed by follow up of the anteroposterior view of the pelvis and bone mineral density has improved. The present case highlights the importance of considering brown tumors in the evaluation of patients presenting with hypercalcemia and osteolytic lesions without definite primary neoplasm.
- The Effect of Fenofibrate and Exercise on Metabolic Syndrome and Hepatic Steatosis in OLETF Rats.
-
Kyung II Lee, Ji Min Kim, Ja Young Park, Ja Won Kim, Ji Young Mok, Mi Kyoung Park, Hye Jeong Lee, Sook Hee Hong, Wenjun Li, Duk Kyu Kim
-
J Korean Endocr Soc. 2007;22(3):192-202. Published online June 1, 2007
-
DOI: https://doi.org/10.3803/jkes.2007.22.3.192
-
-
2,145
View
-
22
Download
-
1
Crossref
-
 Abstract Abstract
 PDF PDF
- BACKGROUND
The aim of this study is to verify the effects of fenofibrate monotherapy and fenofibrate combined with exercise for improving metabolic syndrome and hepatic steatosis. METHODS: Thirty-four weeks old OLETF rats (Otsuka Long-Evans Tokushima Fatty Rats, n = 20) were divided four groups: the regular diet group (n = 5, DD group), the exercise group (n = 5, DE group), the fenofibrate (100 mg/kg) treated group (n = 5, DF group) and the combination treatment group {fenofibrate and exercise (n = 5, EF group)}. After 5 weeks of treatment, blood was drawn for measuring the blood glucose, insulin, lipid and leptin levels. All the subjects were sacrificed for assessment of their body adiposity and hepatic steatosis. RESULTS: The total amount of food intake, body weight and total body weight of the rat were significantly decreased in the EF and DF groups compared to the DD group. The plasma triglyceride and glucose levels were significantly decreased in the EF and DF groups compared to the DD group. The HOMA-IR of EF, DF and DE groups were significantly decreased compared with that of the DD group. The plasma leptin levels of the EF and DF groups were significantly decreased compared with those of the DD and DE groups. The hepatic steatosis index was significantly decreased in the EF and DF groups compared to the DD and DE groups. CONCLUSION: Fenofibrate monotherapy was effective to control three major components (obesity, hypertriglyceridemia and hyperglycemia) of metabolic syndrome and hepatic steatosis in OLETF rats. Exercise combined with fenofibrate treatment showed an additional effect compared to that of fenofibrate monotherapy.
-
Citations
Citations to this article as recorded by  - Effect of Fenofibrate and Exercise on Metabolic Syndrome and Hepatic Steatosis
Bong Soo Cha, Jae Hyuk Lee
Journal of Korean Endocrine Society.2007; 22(3): 188. CrossRef
|